Why Paying $72,000 Made Money
By Markus Grant | The Ranter | Article 3 | The Body Tax
I spent three weeks looking for the mistake. The bureaucratic error. The claims processor who clicked the wrong button. Why does a $72,000 drug get approved in minutes when a $1,900 blood test gets denied as “not medically necessary”?
There’s no mistake. Every decision in the chain does exactly what it’s supposed to do. Make money. For someone who isn’t you.
I followed the money through three different types of insurance. I assumed the trick would change depending on who’s paying. It doesn’t. The plumbing is different. The water goes to the same drain.
The Furnace in the Basement
Before we open the three doors, you need to know what’s running in the basement of every health plan in America. A PBM. Pharmacy Benefit Manager. Three of them -- CVS Caremark, Express Scripts, OptumRx -- control roughly 80% of every prescription filled in this country. Their job is to negotiate drug prices on your behalf. That’s the label on the box.
A drug company wants its $72,000 drug on the approved list. It pays the PBM a rebate -- a percentage of the list price -- for preferred placement. On a $72,000 drug, that rebate runs somewhere between $21,000 and $36,000. Per patient. Per year. And because the rebate is calculated off the LIST price, when the list price goes up, the PBM’s cut goes up too. Both sides make more money when the price is higher. The only person who loses is the one swallowing the pill. This is what happens when you let the bull write the safety manual.
That’s the furnace. It runs the same in every house. Now let’s check who’s paying the heating bill.
Door #1: Your Company Is Self-Insured (And Probably Doesn’t Know It)
Your employer owns the house. They just hired someone else to manage it.
If you work for a company with more than 500 employees, there’s roughly a 65% chance your employer is self-insured. That means your company pays the actual medical bills. The name on your insurance card -- Blue Cross, Aetna, whoever -- that’s not your insurance company. That’s your property manager. They process the paperwork, print the cards, and handle the phone calls. Your employer writes the checks. And separately, a PBM handles the pharmacy side. Who keeps what is decided in contracts your employer usually can’t see.
Your doctor prescribes Humira. $72,000 a year. The claim gets approved. No prior authorization. No delay. The money comes out of your employer’s account.
Your employer sees a “negotiated discount” -- maybe 20% back. $14,400. They think somebody fought for them.
The actual rebate from the drug manufacturer to the PBM? Could be 30-50%. $21,000 to $36,000. Your insurer reports a fraction of it. The PBM keeps its cut. The exact split is in a contract your employer isn’t allowed to read. Trade secret.
Now a different doctor wants to run a $1,900 blood test. No rebate attached to a lab panel. No manufacturer paying a rebate for a diagnostic. Your insurer denies it. “Not medically necessary.”
They’re not paying either bill. It’s your employer’s money. They make more money approving the $72,000 drug -- which generates tens of thousands in rebates -- than approving the $1,900 test -- which generates nothing.
The property manager doesn’t care if the renovation is overpriced. The property manager gets a percentage of the contractor’s invoice.
Door #2: You Bought Your Plan on the ACA Marketplace
Different house. Here the insurer holds the deed. You bought a Silver plan, you pay your monthly premium, and when you file a $72,000 claim, the insurer writes the check. Their money. Not your employer’s.
So they should want to deny it. Right?
Two things stop them. The ACA says they can’t deny you for pre-existing conditions. And the Medical Loss Ratio rule says they must spend at least 80% of premiums on actual medical care. If they don’t, they owe you a refund.
So how does the $72,000 drug make them money?
Because the insurer owns the PBM. UnitedHealthcare pays $72,000 for your Humira. OptumRx -- which UnitedHealth also owns -- collects a $25,000-$36,000 rebate from the manufacturer. That money took the elevator from the sixth floor to the seventh. It never left the building.
And the MLR trick: payments to their own PBM subsidiary count as “medical expenses.” The $72,000 claim satisfies the 80% spending rule even though a massive chunk of it is circulating between departments on the same floor of the same building.
They’re paying themselves rent and calling it a housing expense. Your premium goes up next year -- not just yours, everyone’s in the risk pool. You’re not a cost to this system. You’re a revenue-generating node.
Door #3: Traditional Employer Plan (HMO/PPO Through Work)
You rent. Your employer picked the building. And the landlord already knows what you’re going to cost.
Your company picks an insurer. You split the premium -- employer pays maybe $27,000 a year, you pay $3,900 out of your paycheck. The insurer bears the risk. If you file a $72,000 claim, that’s their problem.
So they should want to keep costs low. They’re the ones paying.
Except the insurer set your employer’s premium LAST year knowing that a certain percentage of employees would end up on expensive drugs this year. Actuaries built that into the rate. Your $72,000 Humira isn’t a surprise. It’s a line item in a projection that was priced twelve months ago.
And the furnace still runs. The insurer contracts with a PBM -- maybe one they own, maybe a partner. The PBM collects $21,000-$36,000 in rebates from the manufacturer. If the insurer owns the PBM, the rebate stays in the family. Net cost after rebates: $36,000-$50,000. Not $72,000.
Next year, the insurer raises your employer’s premium. Your employer passes it to your paycheck. You don’t know why. HR sends an email about “rising healthcare costs.” Nobody mentions the word rebate.
Your rent went up. The landlord won’t show you the books. And every building on the block has the same landlord, could be Blue Cross, could be Aetna, could be United again, doesn’t matter, the furnace is the same.
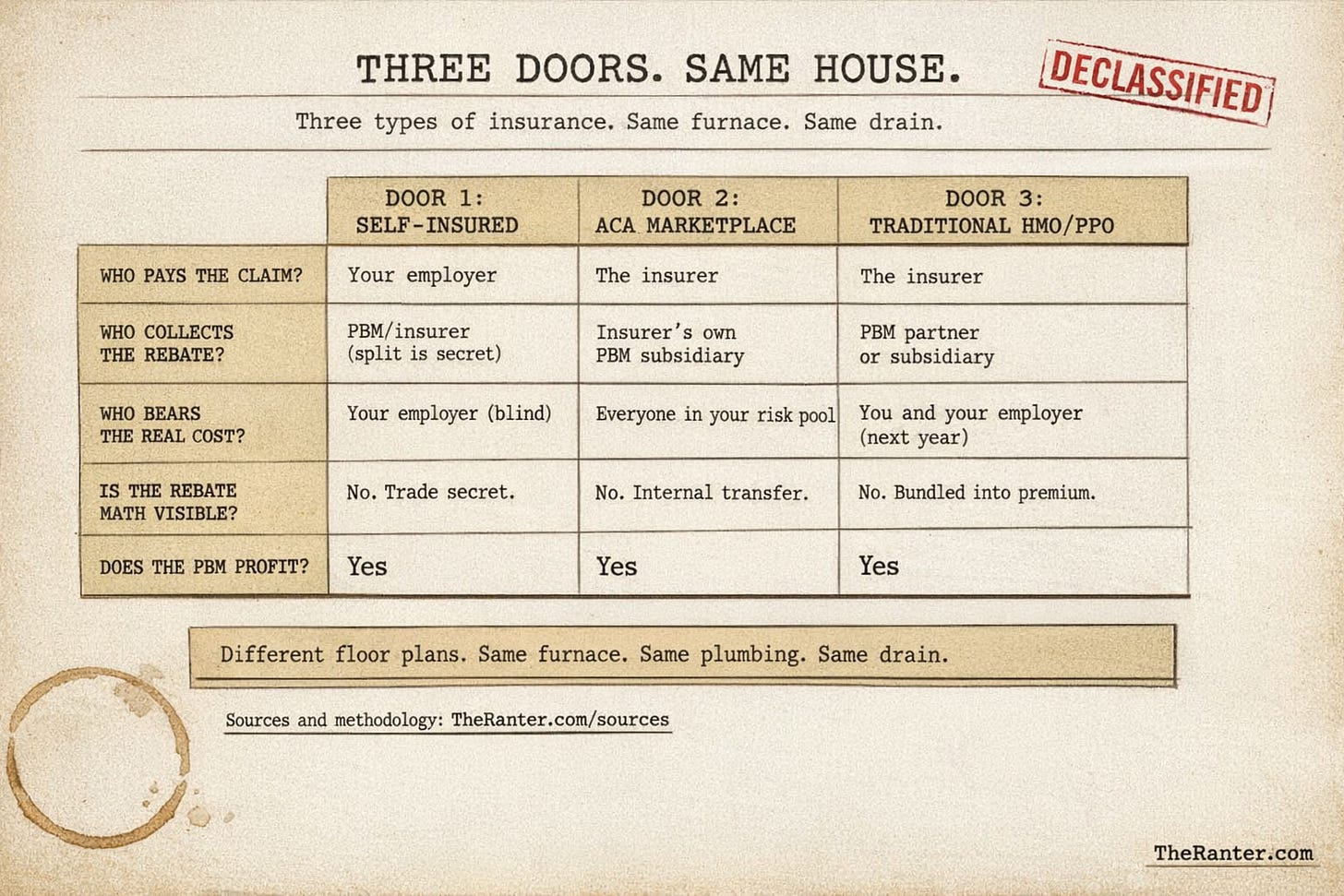
Three Doors, Same House
Three doors. Different floor plans. Same furnace. Same plumbing. Same drain.
The Welcome Mat
My producer stopped me after I finished the three doors.
“They pay $200 a year toward my gym. $100 if I go to the doctor. $100 for the dentist. There’s a mental health line I can call at 3am. They send me emails about drinking water. They gave me a Fitbit. Are you saying that’s fake? Because it doesn’t feel fake.”
It’s not fake. That’s what makes it work.
Your employer pays the claims. A heart attack costs them $200,000 to $800,000. Your gym costs them $200. They want you healthy because you’re cheaper healthy. The gym is real. The checkup is real. Preventive care works. Nobody’s faking that part.
The part nobody mentions is who’s running the program.
Your wellness platform -- the app, the points, the biometric screening -- is usually operated by a subsidiary or partner of the same companies in the chain. Rally Health is UnitedHealth. Virgin Pulse -- now rebranded as Personify Health -- is owned by the same private equity firms that invest across the healthcare industry. Vitality partners with the insurers directly. You’ve probably used one of these platforms. Logged your steps, earned your points, collected your gift card. Did you ever check who was on the other side of the app?
And then think about what a checkup does inside this system. Doctor finds something. Refers you to a specialist. Specialist writes a prescription. Prescription flows through the PBM. The furnace kicks on. That $100 wellness visit that was supposed to keep you OFF medication just became the intake form that puts you ON a $72,000-a-year drug running through the same furnace.
Nobody designed the wellness program to be a funnel. But nobody designed it not to be one, either. The front door is real. The hallway it leads to is the same one behind every other door in this building.
My producer was quiet for a while after that. Then: “They gave me a Fitbit, Markus.”
Yeah. They gave you a pedometer and a pipeline. You just can’t see where the steps lead.
By the way -- UnitedHealthcare runs a program where your Fitbit data gets matched against your medical claims to build predictive health models. The Fitbit wasn’t free. You just didn’t pay for it in cash.
Why Nobody Gets Cured
A cured patient is a closed account. No refills. No rebates. No recurring revenue.
A chronic patient refills every month. Every refill runs through the PBM, generates a rebate, produces a spread. The $1,900 test that finds the real problem? Zero rebate. The system denies it because the test doesn’t pay it back.
A cure is a sale. You close once, the house is gone. A chronic prescription is a lease -- $72,000 a year, renewing automatically, with a landlord who never has to fix anything.
Somewhere around the third spreadsheet, I realized something a comedian figured out on a stage twenty-six years ago. There is no money in the cure. The money is in the medicine. The audience laughed because they recognized it. I’m not laughing. I’m showing you the receipt.
What You Can Actually Do
Door #1 (Self-insured): Ask HR if your company has audited its PBM contract. The DOL proposed a disclosure rule in January 2026. Most employers don’t know they can demand a full rebate audit.
Door #2 (ACA marketplace): Check your formulary. The “preferred” drugs generate the biggest rebates, not necessarily the cheapest. Ask your doctor about therapeutic equivalents off the preferred list.
Door #3 (Through work): When HR emails about “rising healthcare costs,” ask one question: has the company audited its PBM rebate pass-through rate? If the answer is “what’s a PBM,” you found the problem.
For everyone: The math is a trade secret. That’s not a conspiracy theory. That’s a filing system. The house is rigged. But you can still ask to see the blueprints.
SOURCES & RECEIPTS
[1] FTC Interim Report on PBMs (2024, 2025). Big Three control ~80% of prescriptions. Markups of hundreds to thousands of percent on specialty generics. https://www.ftc.gov/reports/pharmacy-benefit-managers-report
[2] Total manufacturer rebates to PBMs: $334 billion (2023). FTC / industry data.
[3] DOL Proposed Rule (January 2026). PBM disclosure for self-insured employers. Estimated savings: up to $1.1 billion annually.
[4] California SB 41 (October 2025). Fiduciary duty on PBMs, 100% rebate pass-through. Challenged in court by PBM industry, January 2026.
[5] KFF. ~30% of Americans skip doses due to cost. U.S. brand prices 422% of OECD peers (list), 308% (net).
[6] AbbVie/Humira: 247 patents. Manufacturing cost estimates under $1,000/year. USPTO / biosimilar industry analysis.
[7] Medical Loss Ratio (MLR) requirements: ACA Section 2718. 80% individual/small group, 85% large group.
[8] UnitedHealthcare/Fitbit data program: Fitbit data analyzed by Qualcomm Life, matched against medical claims to build predictive models. Up to $1,500/year incentive. (GovTech / The Conversation / U.S. News, 2017-2025).
[9] Rock, C. (1999). “Ain’t No Money in the Cure.” *Bigger & Blacker*, HBO. Recorded at the Apollo Theater, Harlem. Available on Max. *Yes, we cite standup specials. If the bit holds up after twenty-six years, it’s evidence.*
**Next:** What happens when you fight back against a denial. And the AI that’s waiting for you when you do. Friday on The Ranter.